
Aortic aneurysms are often called the ‘silent killers’ as patients often experience their first symptoms when the aneurysms rupture. Studies show that nearly 75% of patients with ruptured aneurysms will not survive.
This is exactly the reason why aneurysm awareness, education, and screening are crucial. Ruptured abdominal aortic aneurysms (AAA) are the 15th leading cause of death in the US and the 10th leading cause of death in men over the age of 55. Studies indicate that as many as 5% of men over the age of 60 will have an AAA, and by the age of 80, nearly 10% of men are at risk for developing an AAA. Women, in contrast, typically develop AAAs a bit later at the age of 65 or older.
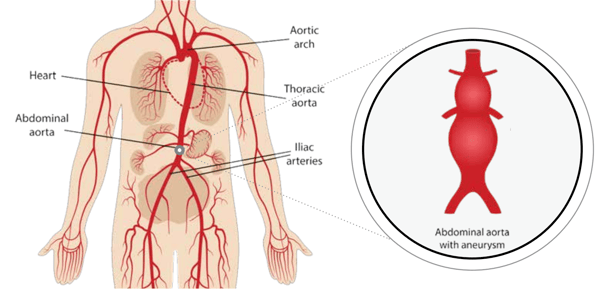
The aorta is the main blood vessel that carries blood from the heart to the rest of the body and is similar in size to a large garden hose. It wraps around the heart and travels down through the chest (where it is known as the thoracic aorta) into the lower abdomen (where it becomes the abdominal aorta). Along the way, the aorta gives rise to blood vessels that supply circulation to all parts of the body. An aneurysm is a progressive weakening and ballooning of a section of the blood vessel wall, and when the blood vessel grows to greater than 1.5 times its normal size, it is called an aneurysm. If undiagnosed and untreated, an aneurysm can rupture, resulting in catastrophic internal bleeding and death.
Knowing the Risk Factors
The risk factors for developing AAA include:
- Older than 60 years of age
- Tobacco use
- Family history of aneurysms
- History of heart disease
- High blood pressure
- Chronic obstructive pulmonary disease
- Peripheral artery disease
 Smoking has been shown as an independent risk factor for developing an AAA. The relative risk of developing an AAA was fivefold higher for smokers than nonsmokers. This risk also rises with the number of years that an individual used tobacco. Aneurysms tend to run in families. First-degree relatives of an individual with an AAA are 3-5 times more likely to develop an AAA. The chance of being diagnosed with AAA is directly related to awareness of its predisposing risk factors. Aortic aneurysms lay in front of the lumbar vertebral bodies and are tucked away behind most abdominal organs. This makes it difficult for physicians to appreciate their pulsatility; hence they are often not recognized on physical examination alone. In patients with various risk factors described above, or in patients with clinical examination that suggests pulsatile abdominal aorta a non-invasive ultrasound examination is recommended for initial evaluation, and depending on aneurysm location a CT scan can offer more detailed information. Far too often aortic aneurysms are only diagnosed accidentally when patients get CT scans or X-ray evaluations looking other abdominal or back problems, and it would be fair to assume that several hundred thousand Americans are walking around with undiagnosed aortic aneurysms.
Smoking has been shown as an independent risk factor for developing an AAA. The relative risk of developing an AAA was fivefold higher for smokers than nonsmokers. This risk also rises with the number of years that an individual used tobacco. Aneurysms tend to run in families. First-degree relatives of an individual with an AAA are 3-5 times more likely to develop an AAA. The chance of being diagnosed with AAA is directly related to awareness of its predisposing risk factors. Aortic aneurysms lay in front of the lumbar vertebral bodies and are tucked away behind most abdominal organs. This makes it difficult for physicians to appreciate their pulsatility; hence they are often not recognized on physical examination alone. In patients with various risk factors described above, or in patients with clinical examination that suggests pulsatile abdominal aorta a non-invasive ultrasound examination is recommended for initial evaluation, and depending on aneurysm location a CT scan can offer more detailed information. Far too often aortic aneurysms are only diagnosed accidentally when patients get CT scans or X-ray evaluations looking other abdominal or back problems, and it would be fair to assume that several hundred thousand Americans are walking around with undiagnosed aortic aneurysms.
The overarching take-home message is simple: The only way to avoid these catastrophic aortic emergencies is to be aware of your risk factors (older than 60 years of age, family history of aneurysms, tobacco use, history of heart disease, high blood pressure, or peripheral arterial disease) that might predispose you to developing an aortic aneurysm, and talk to your doctor about simple, noninvasive tests that can help detect these potential deadly conditions. If an aneurysm is diagnosed, consult with a vascular surgeon about risk factor modification and treatment options, and talk to your family, as aortic aneurysms are hereditary.
This article is a V-AWARE Property. Center for Vascular Awareness, Inc. (www.myvascularhealth.org)








_2.jpg)