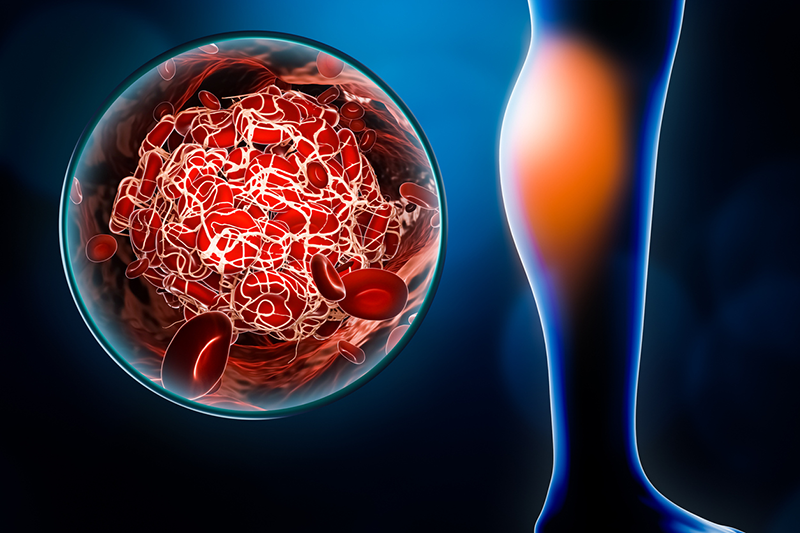
It's already March, and with Daylight Savings just occurring and Spring about to start, it’s also Blood Clot Awareness Month. Blood clots are a common medical condition that can affect us irrespective of age, gender, ethnicity, or race. Not even infants, young children, or teens are immune to this condition.
According to the National Library of Medicine and the Center for Disease Control and Prevention, blood clots affect an estimated 300,000-600,000 individuals in the U.S. each year, causing considerable morbidity and mortality. Seeing how prevalent this condition is, you need to learn as much as possible about it.
Having some basic knowledge of blood clots, especially the two types of clots, is essential to help you seek prompt medical intervention to protect yourself and your loved ones. In this year's Blood Clot Awareness Month, we address the most common concerns and frequently asked questions about blood clots.
What Are Blood Clots?
Blood plays a critical role in keeping you alive. It flows continuously and smoothly in every part of your body during your entire lifetime. However, it's also programmed to shut off to prevent excess blood loss when you're injured.
Blood clots are healthy and can save a life by preventing severe bleeding. Unfortunately, they can also form for the wrong reasons and result in a stroke, heart attack, or similar fatal medical condition. There are two types of blood clots, namely:
Arterial Clot
Arterial clots typically form in the arteries where blood flows away from the heart to vital organs such as the lungs, brain, intestines, kidneys and lower legs. This type of blood clotting prevents oxygen from reaching the lungs and other vital organs and may cause damage to the tissue.
Arterial clots usually form in the legs and feet. In extreme cases, they can form in the brain, resulting in stroke or a heart attack. Arterial clots can also form in your kidneys, eyes, and intestines, albeit a rare occurrence.
Symptoms Of Arterial Clots
The primary symptoms of this type of blood clot may not be evident in the initial stages until it is fully grown hence blocking your normal blood flow. When this happens, you may experience the following:
- Cold limbs
- Cold fingers and hands
- Muscle spasms or pain in the affected area
- Numbness and tingling in your limbs
- Loss of color in the affected area
Venous Clots
Venous clots typically occur in the veins, developing slowly before you start to notice the symptoms.
Three different types of blood clots take place in the veins. They include:
- Superficial venous thrombosis: This blood clot forms in the veins close to the skin surface. While they don't break or flow through your system, they can be extremely painful and require specialized treatment.
- Deep vein thrombosis: DVT is sometimes called venous thrombosis and forms in the more prominent veins deep inside your system. This blood clot usually occurs in the lower leg, pelvis, thigh, and other vital organs, including the brain, kidney, intestines, or liver.
- Pulmonary embolism is the most dangerous blood clot usually treated as a medical emergency. It's a DVT that flows from your leg to your lungs, where it can get stuck and cause death.
Symptoms of Venous Clots
If you have a superficial venous thrombosis where the blood clot is near the skin surface, symptoms usually include:
- Painful and inflamed skin around the affected area
- Painful, tender veins
- Red skin around the affected area
On the other hand, if you have DVT expect any of the following symptoms:
- Swollen and painful legs
- Warm, red and sore legs
- Aching and a heavy feeling on the affected area
This type of clotting is a medical emergency, and you should consult your doctor immediately if you notice such symptoms. Otherwise, it can escalate into a severe pulmonary embolism if left untreated. Call 911 if you notice these symptoms characterized by chest pains, sudden shortness of breath and heavy breathing.
Blood Clots and Traveling: What Should You Do?
If you're diagnosed with DVT, it's advisable to avoid flying due to the risks and complications associated with the condition. For example, there's the risk of the clot breaking free.
Also, traveling by air generally takes at least 4 hours in a sitting position. This is risky and may cause the clot to break and travel to your vital organs, such as the lungs, leading to a heart attack.
It is advisable to consult your doctor if you must travel, especially by plane. Ideally, your doctor may recommend that you wait for at least four weeks from the start of your DVT treatment before flying.
It would help if you continued taking the prescribed medication for blood thinning. Otherwise, consider these tips when traveling after being diagnosed with DVT:
- Wear compression socks
- Stand and stretch every few hours during your flight
- Watch out for symptoms of DVT
- Exercise the calf muscle by doing ankle rolls or standing on your tippy toes to increase blood circulation
- Take blood-thinning medication
- Drink plenty of water to stay hydrated throughout your flight
If you're fitted with an inferior vena cava (IVC) filter to help prevent a pulmonary embolism, it can be removed when the risk of blood clots moving to your lungs has passed. IVC is usually given to people who cannot undergo anticoagulation treatment.
However, if you can take blood thinners, you may not need a IVC filter. But if you must be fitted with one, how long it can stay depends on the severity of the risk factors. Otherwise, your doctor will remove it when it's no longer needed.
Get Professional Help
While blood clotting is a serious medical condition, it's treatable if diagnosed early. Whether you have been diagnosed with DVT or you're experiencing symptoms of possible blood clotting, we can help.
Please schedule an appointment if you’re experiencing any of the symptoms described above or for any vascular or vein condition you might be dealing with.








_2.jpg)